What is Minimally Invasive Laparoscopic Gynaecological Surgery?
Minimally invasive laparoscopic surgery involves making small, keyhole-sized incisions, typically less than 1 cm, in the abdomen. Through these incisions, your doctor inserts a laparoscope (a thin tube with a camera and light) to get a clear, magnified view of the pelvic cavity. Specialised, miniature instruments are then used to operate and perform the procedure without disrupting surrounding tissues.
Unlike traditional open surgery, which requires a large abdominal incision (generally 10-15cm), laparoscopic techniques aim to reduce tissue damage, bleeding, and postoperative pain, while improving aesthetic outcomes and recovery time needed.
Laparoscopic vs. Gynaecological Surgery
| Aspect | Minimally Invasive Laparoscopic Gynaecological Surgery | Traditional Open Gynaecological Surgery |
| Incision size | Keyhole-sized, under 1cm | Larger incisions, typically 10-15cm |
| Scarring | Smaller and minimal scar | Larger surgical scar |
| Pain and discomfort | Less postoperative pain | Higher levels of pain due to larger wounds |
| Downtime | A week or less | Several weeks to months |
| Hospital stay | On the day of the procedure or overnight | Generally 3-5 days |
| Surgical visibility | High-definition camera for a magnified view in real-time | Direct view of the surgical site |
| Infection risk | Lower risk of postoperative complications | - |
| Recommended for | Patients seeking minimally-invasive, fertility-preserving care | Complex cases where laparoscopic access is limited or not feasible |
Dr Tan Heng Hao is trained in laparoscopic gynaecological surgery, and has performed thousands of minimally invasive procedures, such as ovarian cyst and fibroids removal. Most of these are related to infertility conditions.
What conditions can Laparoscopic Gynaecological Surgery diagnose and treat?
Minimally invasive laparoscopic surgery involves making small, keyhole-sized incisions, typically less than 1 cm, in the abdomen. Through these incisions, your doctor inserts a laparoscope (a thin tube with a camera and light) to get a clear, magnified view of the pelvic cavity. Specialised, miniature instruments are then used to operate and perform the procedure without disrupting surrounding tissues.
Unlike traditional open surgery, which requires a large abdominal incision (generally 10-15cm), laparoscopic techniques aim to reduce tissue damage, bleeding, and postoperative pain, while improving aesthetic outcomes and recovery time needed.
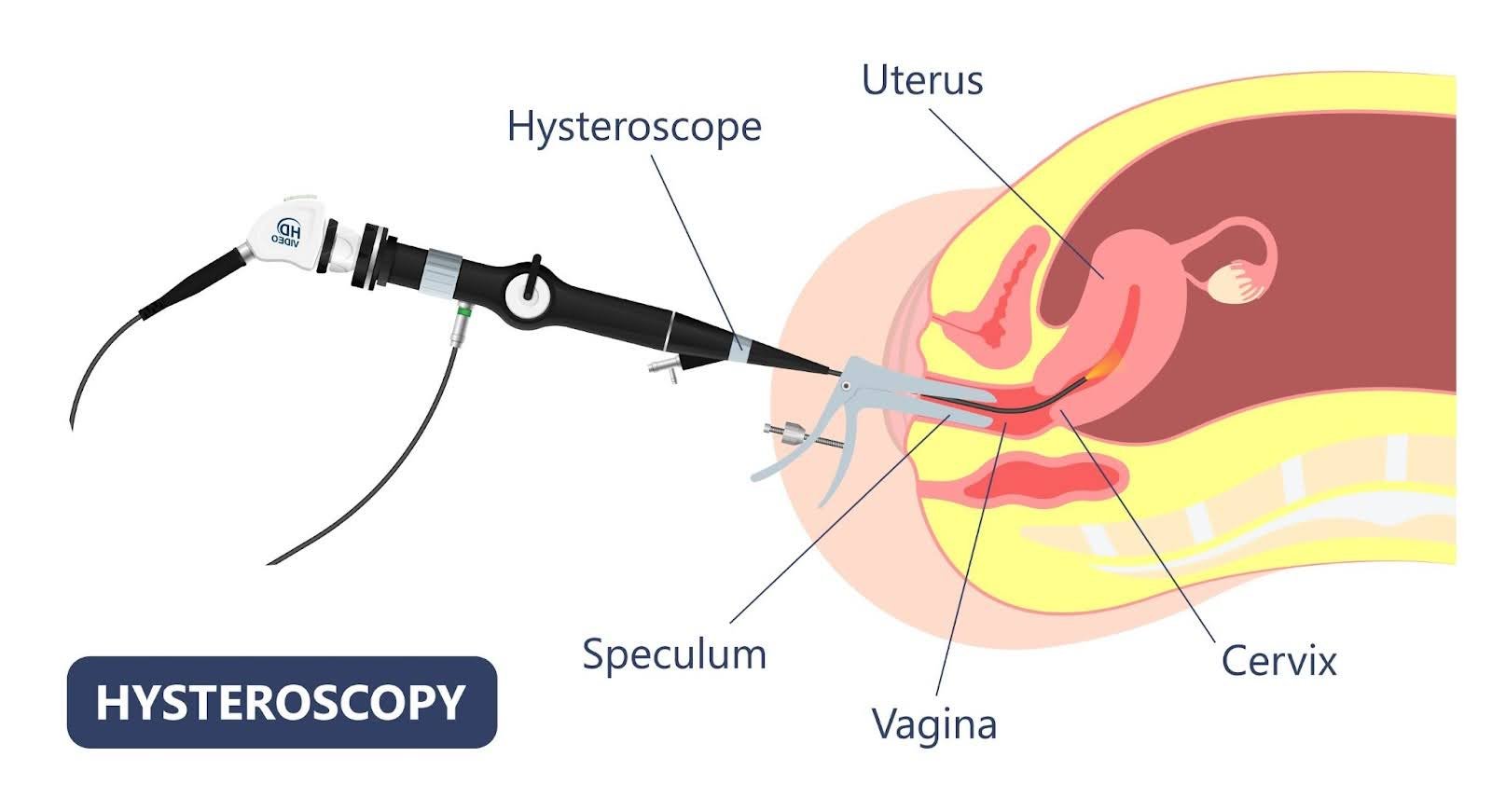
Laparoscopic hysteroscopy is a minimally invasive procedure used to diagnose and treat intrauterine conditions with enhanced precision and reduced recovery time.
Diagnostic use
Laparoscopy allows your gynaecologist to closely examine the pelvic organs for any structural abnormalities, providing useful visualisation when non-invasive imaging does not suffice. It can be used to diagnose and evaluate:
- Pelvic pain
- Endometriosis
- Infertility
- Pelvic adhesions
- Pelvic masses or growths
Sometimes, a laparoscopy is recommended as a second-line diagnostic tool if your doctor picks up something unexpected during your pelvic ultrasounds, MRIs or CT scans. Laparoscopy can also be used to collect tissue samples (biopsy) if required.
Treatment
Gynaecological laparoscopic procedures can be performed as a minimally invasive alternative to traditional surgery for conditions like:
- Ovarian cysts - persistent or painful cysts in the ovaries.
- Uterine fibroids - fibroids that could be causing menstrual and fertility-related issues.
- Endometriosis - endometrial tissue that grows outside the uterus, causing pain or difficulty conceiving.
- Ectopic pregnancy - pregnancies that occur outside the uterus.
- Blocked or damaged fallopian tubes - blocked, twisted or damaged fallopian tubes that can affect lower chances pregnancy and increase risk of an ectopic pregnancy.
- Pelvic adhesions - scar tissue that forms in the pelvic region, causing discomfort and restricting organ movement.
- Ovarian torsion - ovaries that twist around the ligaments, cutting off its own blood supply and affecting ovarian function.
Benefits of Gynaecological Laparoscopic Surgery
Patients often opt for minimally invasive laparoscopic surgery (if possible), as it confers benefits, such as:
- Improved post-procedure cosmesis - as smaller incisions are used, scars are more discreet, heal faster, and have better cosmetic outcomes.
- Faster recovery - smaller incisions also entail a comparatively faster recovery compared to traditional open surgeries.
- Less postoperative pain - minimally invasive surgery causes less disruption to surrounding tissues, which lead to lower pain levels post-op
- Shorter hospital stay - laparoscopic procedures are often day surgeries or only require an overnight stay for observation
- Lower risk of complications - smaller incisions lead to lower risk of complications, such as infection.
- Enhanced visualisation - with 3D, magnified imaging using the laparoscope, your doctor has better visualisation of the operating site, which entails more precision and accuracy.
- Smaller post operative scars - as smaller incisions are used, a minimally invasive gynaecologic surgery leads to smaller and discreet scars
What to expect from Laparoscopic Gynaecological Surgery?
MIS Laparoscopic Gynaecological Surgery at a glance:
| Treatment time | 1-3 hours, depending on the complexity of the procedure |
| Anaesthesia | general anaesthesia (GA) |
| Incision size | keyhole-sized, less than 1cm |
| Hospital stay | day surgery (same-day discharge) or overnight stay |
| Recovery period | generally 1-2 weeks |
| Scarring | minimal and discreet |
| Pain and discomfort | mild to moderate |
Before your procedure
Before your procedure, Dr Tan Heng Hao will conduct a thorough consultation with you to assess your condition, have a thorough diagnosis, and determine your suitability for a laparoscopic procedure. Various tests may be run, such as an ultrasound and blood tests, for a detailed assessment.
You may also be required to fast or avoid certain medications before your procedure.
On the day of procedure
You may be admitted to the hospital where we will prepare you for your procedure. General anaesthesia will be administered to ensure you’re kept as comfortable as possible.
The procedure
Dr Tan Heng hao will make tiny incisions near your belly button. These will be access points for the laparoscope and miniature tools. The procedure will generally last for about 1-3 hours.
Post-procedure and recovery
You may be kept for monitoring in a recovery room for a few hours or overnight. You may experience some bloating or mild discomfort, but this will subside within a few days. Recovery should be generally smooth and relatively quick. Remember to follow your doctor’s aftercare and recovery instructions.
Follow-up appointment
We may schedule a follow-up appointment with you to ensure proper recovery and to address any concerns you may have. Dr Tan will also review your procedure results with you.
Is Laparoscopic Gynaecological Surgery safe?
Generally, laparoscopic gynaecological surgery has a low risk-profile, and is considered safe and effective when performed by a skilled and experienced gynaecologist. However, as with any surgery, and although rare, it does come with its own set of risks and possible side effects, such as:
- Bleeding - you may experience internal or external bleeding during or after the procedure, although rare.
- Infection - there is a risk of infection at the incision sites or internally. This can be prevented with the right surgical practices and proper aftercare.
- Conversion to open surgery - in some complicated cases, a laparoscopic procedure may need to be switched to an open surgery instead.
- Anaesthesia-related complications - general anaesthesia may be administered to put you to sleep during your procedure for a comfortable and pain-free experience. However, in rare cases, patients may experience an allergic reaction or post-op drowsiness.
Before any procedure, your gynaecologist will assess your suitability for the treatment to ensure your safety. Many of these risks can also be prevented by choosing an experienced doctor, and by following the clinic’s aftercare instructions well, attending follow-up appointments, and by giving your body time to rest and heal.
Who is suitable for Laparoscopic Gynaecological Surgery?
Although minimally invasive laparoscopic gynaecological surgery is generally suitable for many, it may not be for some patients. A detailed assessment with your doctor can help determine your eligibility, and it is based on factors, such as:
- Your overall health
- Your body’s receptivity to anaesthesia
- Your gynaecological condition and its severity
- Your body weight being within a manageable range
- The possibility of widespread infection or pelvic inflammation
- Your personal preference
- Any prior abdominal surgeries that may affect laparoscopic entry
Summary
Minimally invasive laparoscopic gynaecological surgery has transformed how we are treated, offering a safer and refined solution for a variety of gynaecological conditions.
If you experience pelvic pain, abnormal periods, or uterine growths, it’s important to speak to your gynaecologist and discuss possibilities of treatment. Schedule a consultation with Dr Tan Heng Hao for a detailed diagnosis and personalised treatment plan.
Frequently Asked Questions
Can all doctors perform minimally invasive gynaecological surgery?
No, not all gynaecology doctors can perform laparoscopic surgery. In Singapore, qualified practitioners are required to undergo specialised training and fellowship programmes on minimally invasive laparoscopic surgery. This ensures that your doctors are well-equipped to perform these MIS procedures safely and effectively.
How long is the recovery period for laparoscopic gynaecological surgery?
How long it takes for you to recover largely depends on each individual’s current condition, healing response, and the specific procedure done. Generally, patients return to their day-to-day activities within 2-3 weeks.
Will laparoscopic gynaecological surgery cause scarring?
You may still experience postoperative scars, as with traditional open surgery. However, as smaller incisions are used, this entails smaller and more discreet scars that fade significantly with time.
Where are incisions usually done?
Usually, laparoscopic gynaecological surgery incisions are made near the navel. This may vary depending on the procedure required.
Can MIS gynaecological surgery be used for cancer treatment?
For certain early-stage gynaecological cancers, laparoscopic surgery may be performed. This depends on your diagnosis and eligibility for the procedure.
Dr Tan Heng Hao 陈行灝
Senior Consultant Fertility Specialist, Obstetrician & Gynaecologist FAMS (Singapore), FRCOG (UK), MMED Singapore (OG)(Singapore), MBBS (Singapore)
Dr Tan Heng Hao is an MOH-accredited IVF specialist in Singapore with extensive experience in reproductive medicine, fertility care and advanced reproductive surgery. He previously led the Department of Reproductive Medicine and the IVF Centre at KK Women’s and Children’s Hospital, where he also served as Director of the National Sperm Bank. His clinical interests include IVF treatments, endometriosis-related infertility and minimally invasive surgery for fertility enhancement. He is among the small number of doctors in Singapore with experience performing laparoscopic tubal reversal surgery.
Dr Tan’s practice centres on personalised fertility care. He incorporates IVF technologies, guides couples through each stage of treatment and prioritises a supportive environment that minimises stress while maintaining privacy.
Book an Appointment
